- Industry Solutions
Industry Solutions
From reshaping the quote to cash process, to transforming engagement with channels partners, to achieving excellence in global product launch, Model N enables digital reinvention with industry-specific solutions that maximize revenue.
- Right block
- Industry Solutions
Industry Solutions
From reshaping the quote to cash process, to transforming engagement with channels partners, to achieving excellence in global product launch, Model N enables digital reinvention with industry-specific solutions that maximize revenue.
- Right block
- Products
Our Products
Model N delivers a platform for business reinvention, empowering companies to maximize revenue as they transform Sales, Marketing, Channels, Finance, and Legal processes.
- Right block
- Services & Support
Services & Support
To ensure you get the most out of your Model N investment Model N provides a complete set of professional Customer Success, Services and Support offerings designed to further your business and IT success.
- Right block
- Resources
- Resources
2026 State of Revenue Report
What’s happening in revenue management and compliance this year?
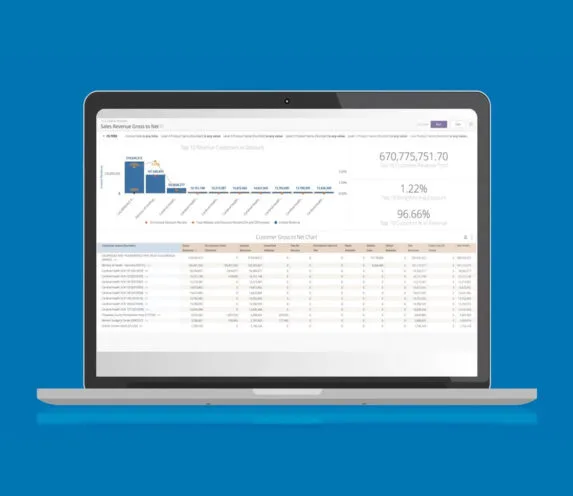
Ninety-six percent of pharma leaders believe that addressing issues early and throughout the gross-to-net lifecycle would materially impact their profit margins. Learn how you can optimize gross to net in 2026.
- Right block
- Resources
- Company
Company
Model N is the leader in revenue optimization and compliance for pharmaceutical, medtech and high-tech innovators. For more than 25 years, we have helped customers maximize revenue, streamline operations, and maintain compliance through cloud-based software, value-added services, and data-driven insights.
- Right block
Contact Sales















 product brief
product brief

 Solution Brief
Solution Brief


.
- Products
Our Products
Model N delivers a platform for business reinvention, empowering companies to maximize revenue as they transform Sales, Marketing, Channels, Finance, and Legal processes.
- Right block
- Services & Support
Services & Support
To ensure you get the most out of your Model N investment Model N provides a complete set of professional Customer Success, Services and Support offerings designed to further your business and IT success.
- Right block
- Resources
- Resources
2026 State of Revenue Report
What’s happening in revenue management and compliance this year?
Ninety-six percent of pharma leaders believe that addressing issues early and throughout the gross-to-net lifecycle would materially impact their profit margins. Learn how you can optimize gross to net in 2026.
- Right block
- Resources
- Company
Company
Model N is the leader in revenue optimization and compliance for pharmaceutical, medtech and high-tech innovators. For more than 25 years, we have helped customers maximize revenue, streamline operations, and maintain compliance through cloud-based software, value-added services, and data-driven insights.
- Right block
- Industry Solutions
Industry Solutions
From reshaping the quote to cash process, to transforming engagement with channels partners, to achieving excellence in global product launch, Model N enables digital reinvention with industry-specific solutions that maximize revenue.
- Right block
- Products
Our Products
Model N delivers a platform for business reinvention, empowering companies to maximize revenue as they transform Sales, Marketing, Channels, Finance, and Legal processes.
- Right block
- Services & Support
Services & Support
To ensure you get the most out of your Model N investment Model N provides a complete set of professional Customer Success, Services and Support offerings designed to further your business and IT success.
- Right block
- Resources
- Resources
2026 State of Revenue Report
What’s happening in revenue management and compliance this year?
Ninety-six percent of pharma leaders believe that addressing issues early and throughout the gross-to-net lifecycle would materially impact their profit margins. Learn how you can optimize gross to net in 2026.
- Right block
- Resources
- Company
Company
Model N is the leader in revenue optimization and compliance for pharmaceutical, medtech and high-tech innovators. For more than 25 years, we have helped customers maximize revenue, streamline operations, and maintain compliance through cloud-based software, value-added services, and data-driven insights.
- Right block
Quick Links
- Products
- Life Science - MedTech
- Provider Management
Provider Management
Gain real-time visibility and insights into your commercial contracting process to reduce revenue leakage and ensure contract compliance.
View Product BriefManaging GPOs, IDNs, and agreements with healthcare providers is a cumbersome, manual process
- Spreadsheets and siloed, aging systems make tracking customer purchasing behavior and price-tier commitments difficult.
- A lack of visibility can impact your ability to make informed business decisions, correctly calculate chargebacks, validate sales and ultimately protect your bottom line.

How Model N’s Provider Management solution helps you
With Provider Management, you can administer accurate pricing and chargebacks, ensure compliance to price-tier commitment and mitigate rebate overpayments.
Improved margins
Proactively address customer purchasing behavior to ensure they meet their contract commitments.
Reduced risk
Monitor contract net prices daily or on-demand to identify and prevent possible regulatory compliance issues.
Better collaboration
Coordinate back and front office information to create advantageous contracts and ensure compliance.
Clean first-pass rates
Accurately calculate all types of rebates, fees, chargebacks, distributor commissions, and accruals to reduce churn and protect provider revenue stream.
98 %
With clean, accurate data in a single solution, manufacturers can reach greater than 98% clean first-pass rates in processing chargebacks in accordance with Healthcare Distribution Alliance (HDA) best practices
Some of our customers






Looking for more information?
Interact seamlessly with your providers
Model N Provider Management helps you effectively manage and execute the thousands of institutional contracts you have – so you can ensure feasibility and profitability.
Contract and price management
Define and update all pertinent details of your contracts (e.g., effective dates, eligible products and pricing, rebates, customer eligibility, terms and conditions).
Advanced member management
Model N’s new Advanced Membership Management (AMM) module provides streamlined roster import process with reusable mapping sets and data transformations, smart matching utilizing complex algorithms to identity matches and assign members, and instantly publish to Model N’s Provider Management application and assign eligibility for pricing, compliance and rebates and fees.
Federal supply schedule compliance
Track entities, monitor prices, manage and resolve violations, and adhere to request for modification (RFM) policy and processes.
ERP integration
Ensure customers get the right price the first time with real-time integration into your order and billing systems.
Contract compliance
Review customer purchasing activities at any point in time to determine whether they are meeting contract commitments.
Rebate management
Track, validate, and accurately process from simplest to most complex rebates, incentives, fees, and accruals.
Streamline and automate your entire revenue management process

Model N Provider Management is a core component of Model N’s Revenue Cloud, a suite of the most comprehensive solutions to address the needs of life sciences companies.
- End revenue leakage in provider contract pricing and rebating processes.
- Optimize 100% of your global revenue with detailed visibility across all channels.
- Ensure adherence to complex government pricing regulations.
- Provide more strategic incentives in the provider channel.
- Quickly and easily adapt to industry changes.

Add On's
Related products
Related Resources


North America Provider Management
Efficiently manage provider contracts and compliance VIEW product brief

Payer Management Solution Brief
Prevent costly errors and overpayments within payer contracts VIEW Solution Brief
Powering Innovators
Enabling our Customers to Deliver Life-Changing Products to the World
Contact Sales
Thank you for your interest in Model N. Please submit the form and our sales team will contact you within 24 hours.
Our Customers Include:

Thank you for reaching out.
We look forward to responding within one business day.